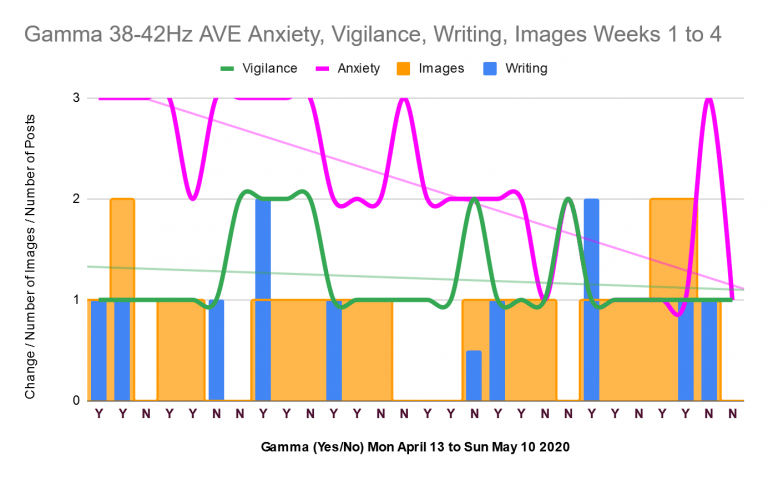
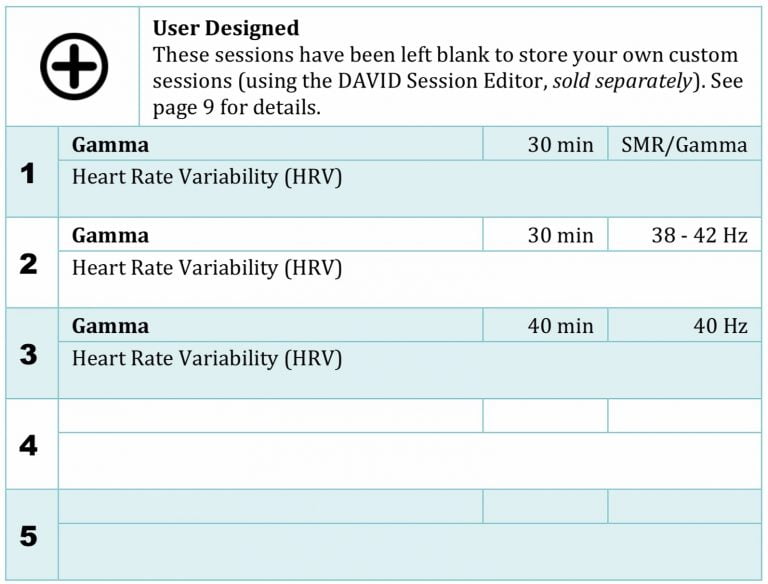
On 13 April 2020, I began a single subject study into audiovisual entrainment of gamma brainwaves at 38 to 42Hz. The ideal gamma brainwave frequency one wants is 40Hz. I finished it yesterday, 10 May 2020. Today, I present the results of four weeks of this study. Results I measured the effect of gamma 38…
Tag: Emotions
Gamma 38 to 42Hz Week Four Progress
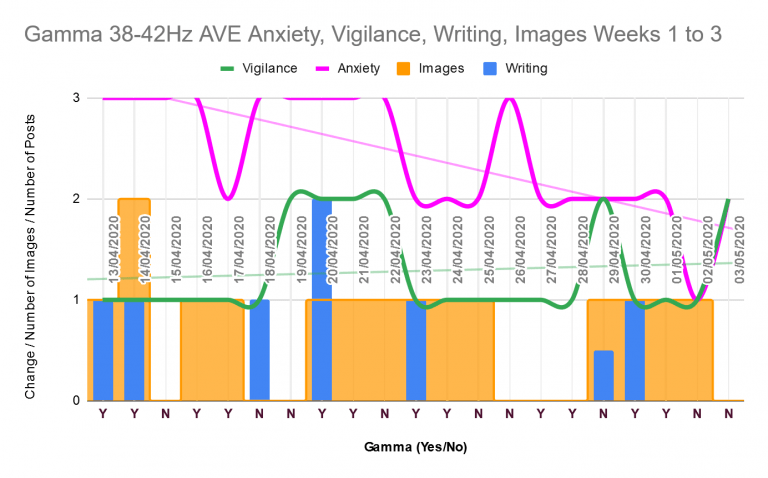
Gamma 38 to 42Hz Week Three Progress
Fatigue walloped me in week three. I struggled with it, and it prevented me from doing what I had the initiation (from gamma) and plans to do. This kind of setback is normal for my brain injury. Any time I think I’m getting somewhere, fatigue rises up like a monster, claws extended, and lands on…
Gamma 38 to 42Hz AVE Week Two Progress
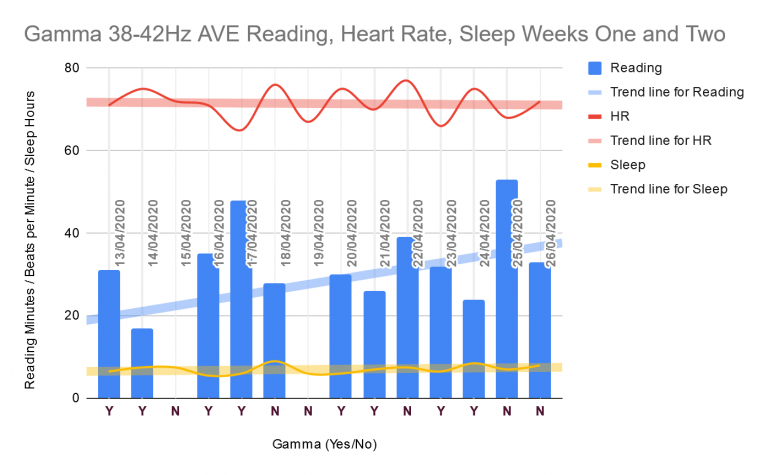
Week one of gamma 38 to 42Hz AVE (audiovisual entrainment) a good start to my single-subject study to see if AVE can replace gamma-brainwave training via brain biofeedback during COVID-19. Week Two:
Gamma 38 to 42Hz AVE Week One Progress
See my post Gamma 38 to 42Hz Audiovisual Entrainment for Brain Injury, Single Subject Study for hypothesis and methodology of this one-month study to see if gamma brainwave audiovisual entrainment will improve functionality and decrease anxiety and vigilance during COVID-19.
Gamma 38 to 42Hz Audiovisual Entrainment for Brain Injury, Single Subject Study
Introduction In 2012, following my inclusion in and subsequent exit from a drug trial that increases GABA in the brain, the ADD Centre, working with me, demonstrated that brain biofeedback of 39 to 42Hz at CZ can increase gamma brainwaves and effect radical improvement in a person with brain injury. You can find the research…
Third SMR/Gamma Mind Alive Session
This morning, my body entered deep relaxation for a few minutes during my usual SMR/Beta audiovisual entrainment session. That normally doesn’t happen. Huh. Does this change support my theory of gamma brainwaves I posited in my book Concussion Is Brain Injury: Treating the Neurons and Me? My brain is settling down into this new audiovisual…
Ground Hog Day?
BrainGirlAndCat does video blogging. She used to be on Twitter, and I came to know her through BIST, I think. The Brain Injury Society of Toronto recently tweeted out her latest video. BIST (@BrainInjuryTO) 2019-07-08, 9:45 AM “Every day is like Ground Hog Day,” From her home in Ireland, Brain Girl shares the story about…
Divorce Is A Scream
Divorce is a scream. A scream of one ignited by the unhappiness of the other one looking for salve elsewhere instead of within the two as promised before the reverend in the time when the two joyously united to each other, together. That’s the problem with divorce. Marriage requires both to permit it. Divorce thuds…